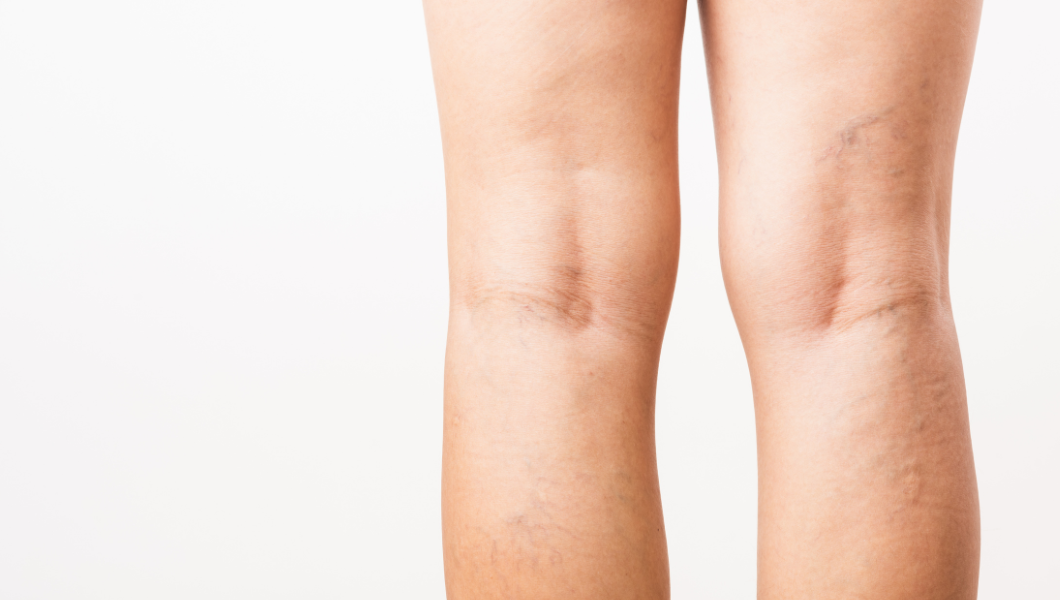
It’s impossible to predict who will or won’t develop them but there are several factors that are proven to increase the risk of varicose veins. While some of these risk factors are beyond your control, others can be influenced by you and your lifestyle choices. This means that there are steps you can take to reduce the risk of varicose veins:
1: Varicose Veins Are In The Family
There’s not much you can do about this one but family history plays a role in the risk of varicose veins because there is a genetic component to the condition. If your parents or close relatives have varicose veins, you have a higher likelihood of developing them yourself. The specific genes responsible for varicose veins have not been fully identified and it is believed that multiple genes may be involved.
2: Age Is A Factor
As we get older, the veins in our legs can gradually lose their elasticity and become weaker. This can lead to the development of varicose veins or worsen existing ones. The aging process can also contribute to other factors that increase the risk of varicose veins. For example, as we age, the valves in our veins may become less effective in regulating blood flow, allowing blood to pool and veins to stretch. Additionally, over time, the wear and tear on our veins from daily activities and lifestyle factors can accumulate, further increasing the risk of varicose veins.
3: Gender Risk Of Varicose Veins
Whilst varicose veins are certainly more commonly associated with women, men are also susceptible to developing them. It is generally estimated that varicose veins affect about 25% to 33% of adult women compared to approximately 10% to 20% of adult men. The increased risk of varicose veins in women is due to such factors as hormonal changes during pregnancy and menopause, as well as the use of hormonal contraceptives. Additionally, female hormones can weaken vein walls and contribute to the development of varicose veins. The risk of varicose veins in men tends to be more genetic and lifestyle related.
4: Pregnancy Increases The Risk Of Varicose Veins
During pregnancy, there are several physiological changes that can contribute to the development of varicose veins during pregnancy:
- Hormonal Changes: Pregnancy hormones, specifically progesterone, can relax the walls of the blood vessels, including the veins. This relaxation can lead to the veins becoming more dilated and prone to becoming varicose.
- Increased Blood Volume: During pregnancy, the body produces more blood to support the growing fetus. The increased blood volume puts additional pressure on the veins, especially in the lower extremities, which can impair the proper circulation of blood and lead to the formation of varicose veins.
- Uterine Pressure: As the uterus expands with the growing fetus, it can exert pressure on the veins in the pelvic area, particularly the inferior vena cava, which is the large vein responsible for returning blood from the lower body to the heart. This pressure can further impede blood flow and contribute to the development of varicose veins in the legs.
- Weight Gain: Pregnancy often involves weight gain, which can put extra stress on the veins and increase the likelihood of varicose vein formation.
It’s important to note that while pregnancy increases the risk of varicose veins, they often improve or resolve on their own after childbirth.
5: Prolonged Sitting Or Standing Doesn’t Help
Prolonged sitting or standing can contribute to the development of varicose veins, but it is not the sole cause. These positions can exacerbate existing vein issues or increase the risk of developing varicose veins in susceptible individuals. Here’s how prolonged sitting or standing can affect vein health:
- Blood Pooling: When you sit or stand for extended periods without movement, blood can pool in the veins of your legs. This is because the muscles responsible for helping to pump blood back to the heart are not actively contracting, impeding the efficiency of blood circulation. As a result, the veins may become dilated and varicose veins may form.
- Increased Pressure: Both sitting and standing can increase the pressure on the veins in your legs. Sitting can restrict blood flow due to the compression of veins by the chair or seat, while standing for long durations can cause blood to accumulate in the lower extremities due to gravity. The increased pressure on the veins can weaken the vein walls and valves, leading to varicose vein development.
- Lack of Muscle Contraction: Physical activity, including regular muscle contractions, plays a crucial role in maintaining healthy blood circulation. When you are sitting or standing for prolonged periods, the lack of muscle movement reduces the pumping action that helps return blood from the legs to the heart. This can contribute to blood pooling and the development of varicose veins.
While prolonged sitting or standing alone may not be the primary cause of varicose veins, it can certainly be a contributing factor
6: Obesity And The Risk Of Varicose Veins
Obesity is considered a risk factor for varicose veins. Excess weight can increase the pressure on the veins in the lower extremities, making it harder for the blood to flow efficiently back to the heart. This increased pressure can lead to weakened vein walls and valves, contributing to the development of varicose veins.
Several ways in which obesity can impact vein health and increase the risk of varicose veins include:
- Increased Pressure: Excessive body weight puts additional pressure on the veins, particularly in the legs. This added pressure can strain the vein walls and valves, impairing their function and leading to varicose veins.
- Impaired Circulation: Obesity can hinder proper circulation as it can affect the overall blood flow throughout the body. Sluggish circulation can contribute to blood pooling and increase the risk of varicose veins.
- Inflammation and Hormonal Changes: Obesity is associated with chronic low-grade inflammation and hormonal imbalances. These factors can negatively impact vein health and contribute to the development of varicose veins.
- Lifestyle Factors: Obesity often goes hand in hand with a sedentary lifestyle and lack of physical activity. Physical inactivity can hinder the muscle contractions necessary for proper blood circulation, further increasing the risk of varicose veins.


7: Lack Of Exercise Increases The Risk Of Varicose Veins
A lack of exercise certainly can increase the risk of varicose veins. Regular exercise and physical activity play a crucial role in maintaining healthy circulation and vein function. When you engage in physical activity, the muscles in your legs contract, which helps pump blood back to the heart against gravity. This muscle contraction promotes efficient blood flow and reduces the risk of blood pooling in the veins.
A sedentary lifestyle, characterized by a lack of exercise or prolonged periods of inactivity, can contribute to the development of varicose veins. Here’s how a lack of exercise can impact vein health:
- Weakened Muscle Pump: Regular exercise, particularly activities that involve leg movement, helps strengthen the calf muscles. These muscles play a key role in pumping blood from the legs back to the heart. Without regular exercise, the muscle pump becomes weaker, which can impede blood circulation and increase the risk of varicose veins.
- Sluggish Blood Flow: Physical activity encourages faster blood flow and prevents blood from pooling in the veins. In contrast, a sedentary lifestyle can lead to sluggish blood flow, which can contribute to the formation of varicose veins.
- Weight Gain: Lack of exercise often coincides with weight gain or obesity, which is a known risk factor for varicose veins. Excess weight can put additional pressure on the veins, making it harder for blood to circulate efficiently.
8: Medical History And The Risk Of Varicose Veins
Prior history of blood clots and certain previous medical conditions can increase the risk of varicose veins. Here are some examples:
- Deep Vein Thrombosis (DVT): Having a history of deep vein thrombosis, which is a blood clot that forms in the deep veins, can increase the risk of developing varicose veins. DVT can cause damage to the valves in the veins, leading to chronic venous insufficiency and the development of varicose veins.
- Superficial Vein Thrombosis (SVT): Similar to DVT, a history of superficial vein thrombosis, which is a blood clot that forms in the superficial veins close to the skin, can also increase the risk of varicose veins. SVT can cause inflammation and damage to the veins, contributing to the development of varicose veins.
- Pelvic Congestion Syndrome: Pelvic congestion syndrome is a condition characterized by varicose veins in the pelvic region, which can lead to pelvic pain and discomfort. Women with a history of pelvic congestion syndrome may be more prone to developing varicose veins in other parts of the body, such as the legs.
- Chronic Venous Insufficiency (CVI): Chronic venous insufficiency is a condition where the veins are unable to efficiently return blood to the heart, leading to blood pooling and the development of varicose veins. Having a history of CVI increases the likelihood of developing varicose veins.
- Post-thrombotic Syndrome: Post-thrombotic syndrome is a complication that can occur after a deep vein thrombosis. It can result in chronic venous insufficiency and the development of varicose veins.
Varicose Veins – It’s Not A Given!
It’s important to note that while these factors increase the risk of varicose veins, they do not guarantee that you will develop them. That said adopting healthy lifestyle habits, such as exercising regularly, maintaining a healthy weight, and avoiding prolonged sitting or standing, you can help reduce your risk. Topical creams such as Venorex Varicose Veins Cream are also thought to help in the prevention of varicose veins.
If you have concerns about varicose veins or notice symptoms, it’s advisable to consult with a healthcare professional for evaluation and appropriate management.